Injury
Ouch! You burned your hand while taking the hot pan off the stove. You slipped on the ice, and your shoulder is aching. You were playing sports and were injured. You woke up pretty sore from your surgery.
These are all examples of acute pain — pain that usually comes on suddenly and goes away when its cause is found and treated or after the body has had time to heal. Although you try to avoid pain, it’s a useful sensation — a warning. Pain tells you that something is happening to your body — that you may need stay off your feet, let go of that hot pan, get to the hospital and deliver that baby, or rest while you recover from your surgery.
But that doesn’t mean you have to endure the pain for long.
Anesthesiologists work with patients and their other doctors to help diagnose pain and treat it safely, effectively, and with as few side effects as possible.
Anesthesiologists can help you. They are medical doctors who treat pain, specializing in anesthesia, pain management, and critical care medicine. Anesthesiologists work with patients and their other doctors to help diagnose pain and treat it safely, effectively, and with as few side effects as possible. They can develop a care plan consisting of prescription and over-the-counter medications, and nonmedication treatments such as massages and physical therapy.
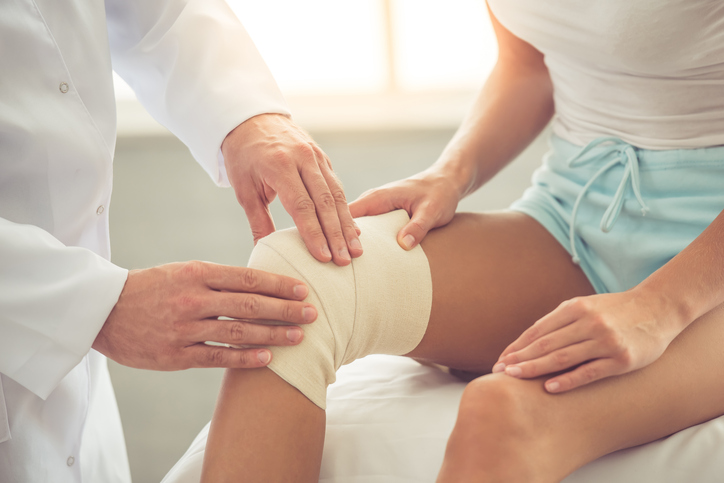
How is acute pain different from chronic pain?
Pain is generally considered acute when it lasts fewer than three months. Acute pain typically starts suddenly in response to an injury — a cut, bruise, burn, broken bone, or pulled muscle, for example. Acute pain can also be caused by a fever or infection, labor contractions, and menstrual cramps.
Pain that lasts for three months or longer is considered chronic pain and can be caused by conditions such as arthritis, back problems, shingles, migraines, and neuropathy (a condition that can result from diabetes and cause numbness or tingling, pricking sensations or muscle weakness).
Sometimes acute pain becomes chronic. A sports injury that isn’t diagnosed and treated properly can lead to long-term damage to joints or muscles. Certain injuries can cause nerve damage that leads to ongoing pain. Even postoperative pain that isn’t managed correctly can lead to chronic pain. So, it’s important that acute pain be accurately diagnosed and effectively treated.
How is acute pain treated?
Often acute pain can be managed with over-the-counter medications such as aspirin or acetaminophen. A sprained ankle or other minor musculoskeletal injury will often respond well to RICE therapy: rest, ice, compression, and elevation. Topical pain medications can also be used for certain types of injuries.

Sometimes acute pain requires more powerful treatments such as opioids, medications that prompt the release of dopamine — a chemical in the brain that reduces the perception of pain. Opioids, such as fentanyl, oxycodone, and morphine, are often needed to manage the pain caused by a major surgery, such as a knee replacement, or a traumatic injury, such as a serious burn or broken bone. It’s important that an anesthesiologist be involved in pain management plans requiring opioids because of the potential side effects and the risk of addiction.
Acute pain is common in children and teenagers who are injured while playing sports. Anesthesiologists use many of the same treatments for these young patients, prescribing opioids only when other treatments aren’t working — and with close supervision.
There are many ways other than medication to manage pain, and anesthesiologists can advise patients and consult with their other physicians and health care providers to develop a care plan. For example, an anesthesiologist may work with a physical therapist to coordinate physical therapy for a patient’s sports injury, or he or she may consult with an oncologist to help manage pain caused by a patient’s cancer or cancer treatment.
Anesthesiologists also can advise patients on the use of therapies such as massage and biofeedback.
